Automated SOAP Notes
AI dynamically structures and generates notes based on diagnosis type, symptoms, and case severity.
Case Study
Reinventing healthcare with Bonami
Client Profile
Multi-specialty healthcare network across inpatient, outpatient, and telehealth practices.
Engagement Focus
Create a self-learning PMS spanning documentation, billing, claims, imaging, and virtual care.
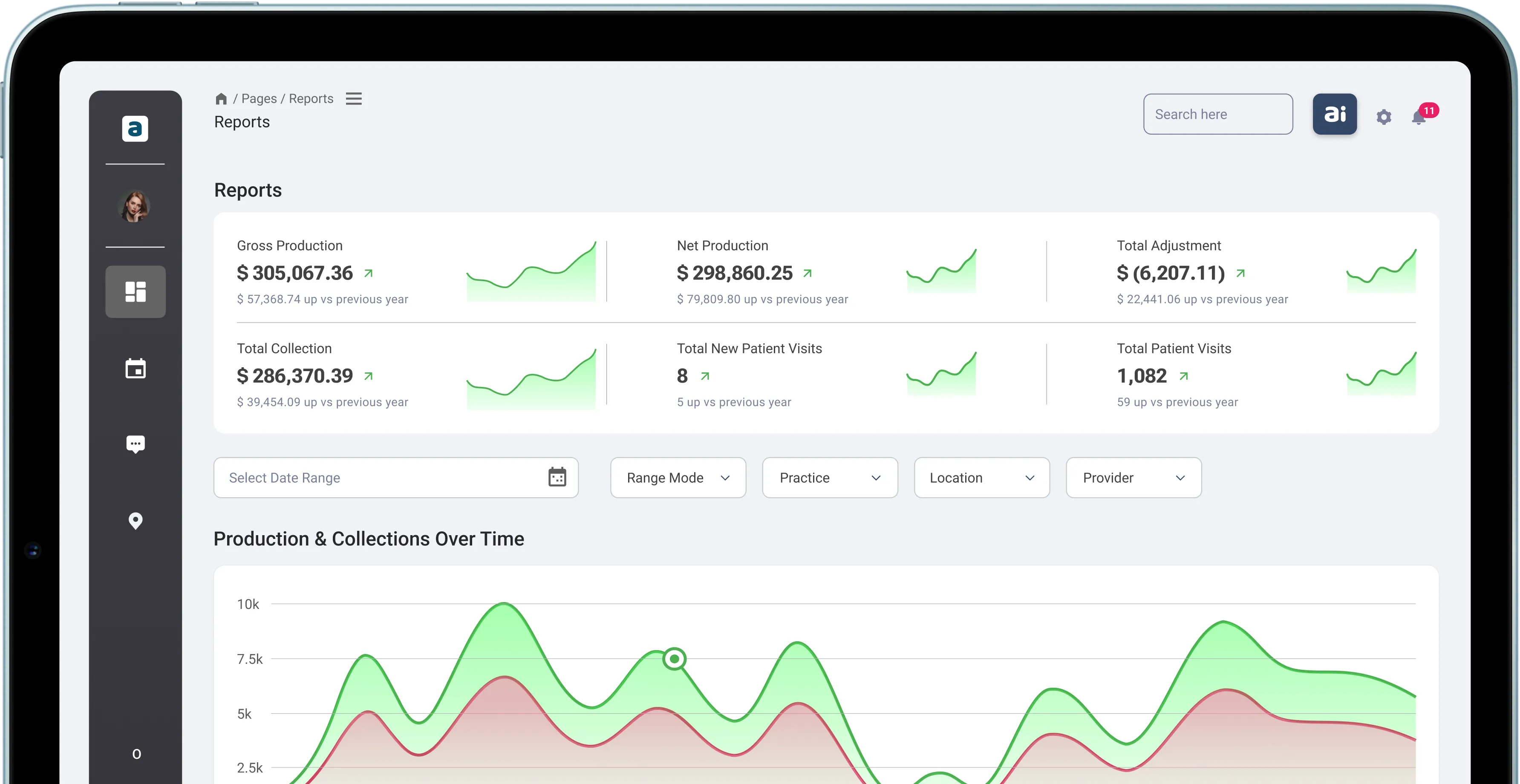
The Challenge
The client’s existing EHR system lacked interoperability and automation, resulting in:
Lengthy SOAP note creation (15–20 mins per visit)
Fragmented billing across departments and insurers
Manual code searches prone to claim denials
Disjointed data across imaging, forms, and teleconsultations
Limited predictive insight into claim aging and patient risk
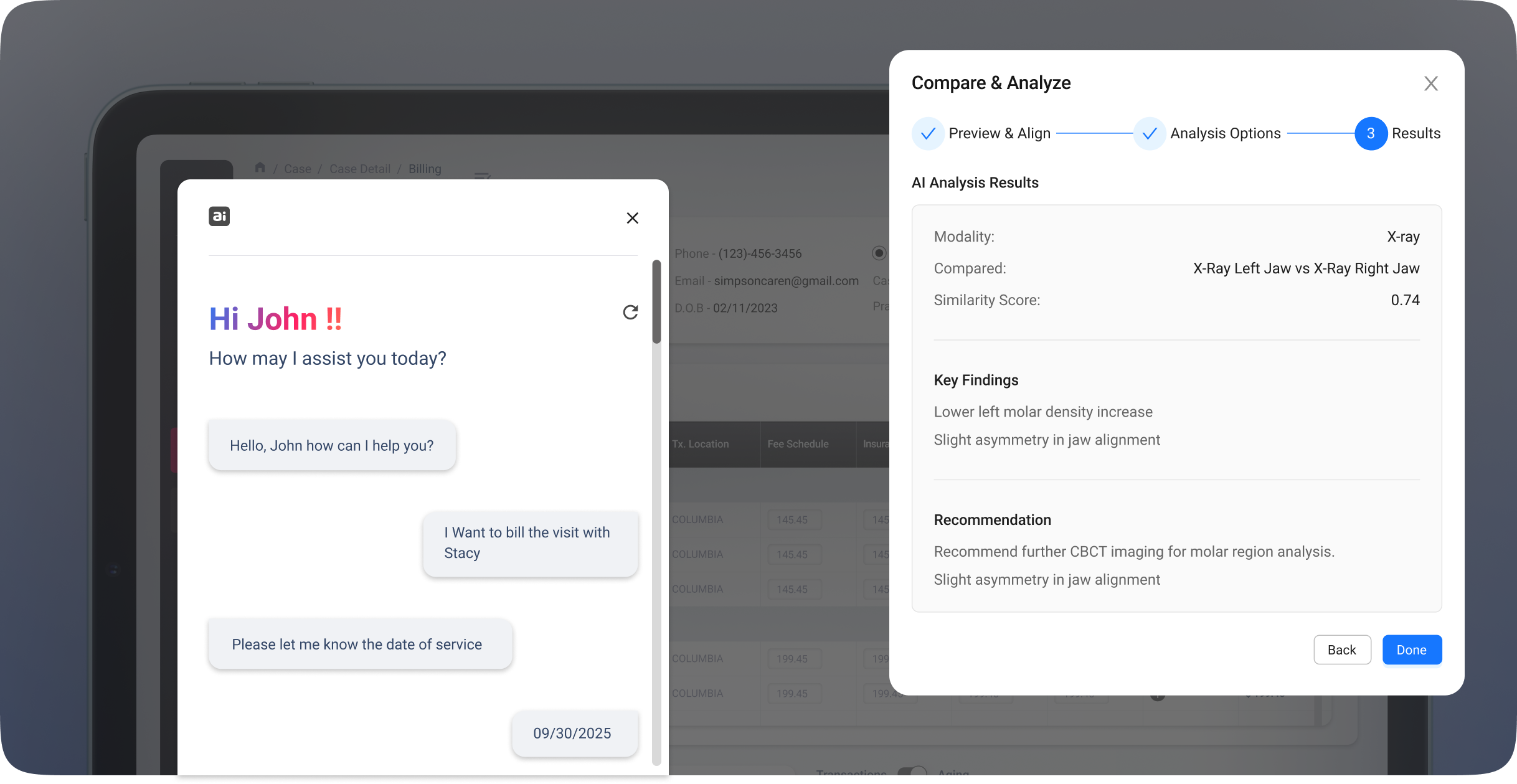
The Solution
AI dynamically structures and generates notes based on diagnosis type, symptoms, and case severity.
Converts simple phrases like “Send John’s bill for today’s visit” into automated, coded invoices.
Contextual retrieval across 100K+ ICD-10 & CPT codes ensures frictionless claim submission.
150+ forms (20–25 pages each) digitized with adaptive field detection and dynamic recognition.
Models claim aging, insurer patterns, and follow-up probabilities using historical data.
Detects anatomical variances across X-rays and reports for clinical review and next-step suggestions.
Context-aware assistant routes users directly to relevant modules like “claims”, “consults”, or “imaging”.
AI-generated call briefs with follow-up recommendations and referral nudges.
Each layer of intelligence continuously learns from provider behavior to make every interaction faster, more accurate, and context-aware.
Experience Re-Imagined
The Impact
0%
Charting Time
~20 min/visit → ~6 min/visit
0%
Claim Accuracy
60–65% → 85%+
0%
Claim Turnaround
5–7 days → 2–3 days
0×
Provider Throughput
1.2x baseline → 2.4x throughput
“Our clinicians now finish documentation before the next patient walks in.” — Medical Director, Partner Clinic
Design Philosophy
Technology Stack
Key Takeaways